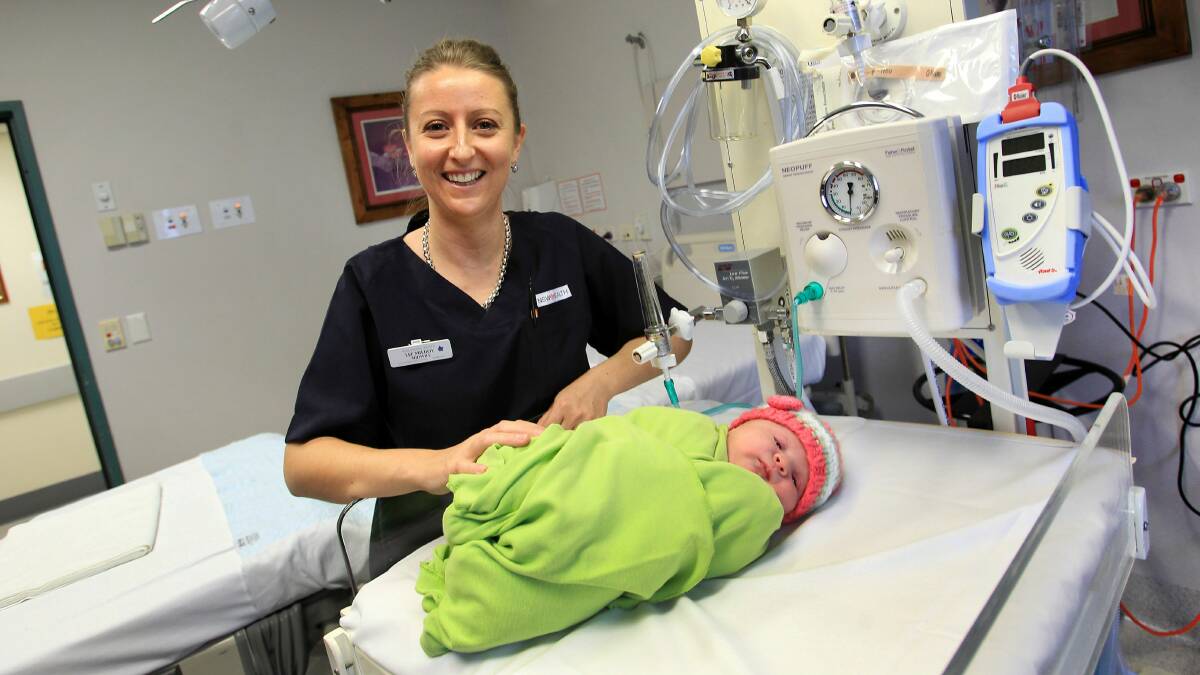
Wollongong's Liz Milroy has been a midwife for 10 years, but nothing could have prepared her for her six-month stint at a basic birthing unit in Bougainville.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
From helping to save the life of a premature baby weighing just one kilo, to attending to the wounds of a woman attacked by her husband with a machete - Ms Milroy still gets tears in her eyes when she reflects on her experience.
She was tasked as a midwife to the Buin Health Centre from October 2012 to April this year as her first posting with the international medical and humanitarian organisation Medecins Sans Frontieres (MSF), also known as Doctors Without Borders.
"Women face so many challenges throughout pregnancy and childbirth - just to get to the health centre warranted a two- to three-hour walk for most of them," she said. "Those who needed caesareans then faced a seven-hour drive on a dirt road in a 4WD to the nearest hospital at Buka. Those who deliver at the health centre do so without any drugs, basic facilities and very limited technology - there's no ultrasounds, no CTG monitoring, no pathology services."
What the local nurses lacked in technology, they made up for in traditional skills and care, said Ms Milroy, who is now back working at Wollongong Hospital's birthing unit.
"They are very skilled at what they do, with the tools that they have available to them," she said.
"They listen to the foetal heartbeat with a pinnard, which is a bell-shaped tool, and they use their hands to feel for the baby's position."
However, the lack of technology meant the lives of some babies and women were inevitably lost.
"There were many upsetting cases - stillbirths and babies who passed away after a few days of life, babies who would have survived if they'd been born in Australia," Ms Milroy said. "And the really sad thing is that women don't even expect all their babies to live."
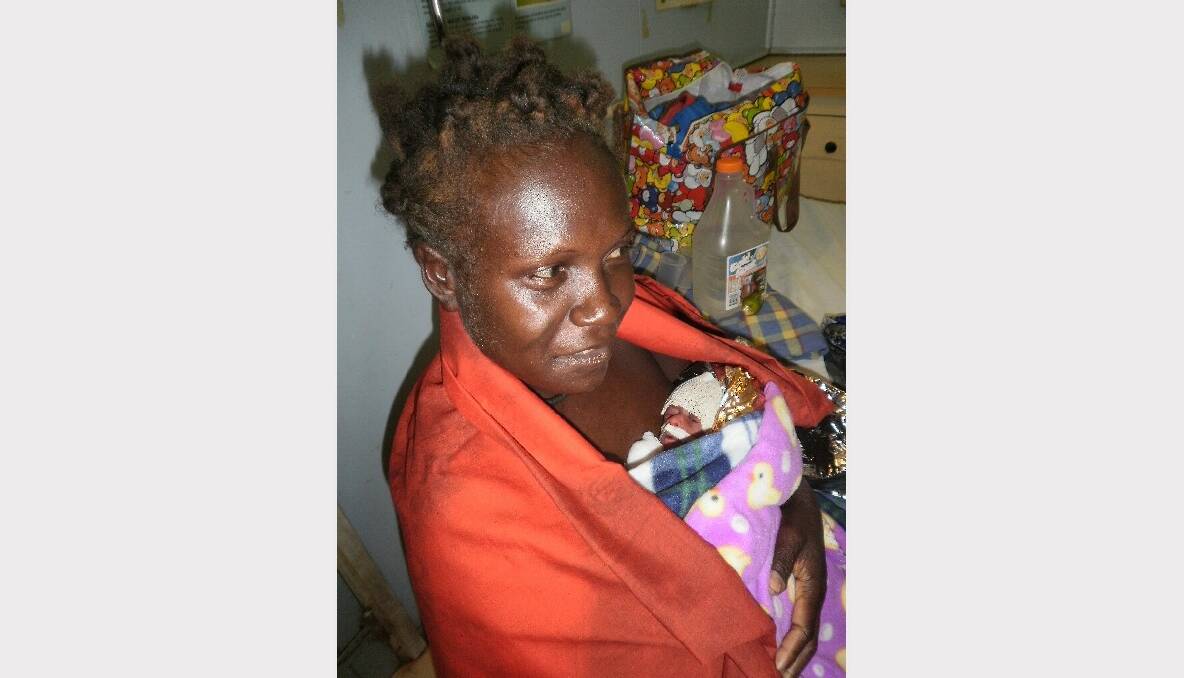
Ms Milroy, and the other doctors and nurses from MSF, were able to help save lives - including that of a special little girl, initially named One Kilo.
"One Kilo came to us on a Sunday afternoon. Her mother, Leanne, had had her 10-weeks early in her village and had carried her for 1½ hours on her walk to the health centre," she said.
"She weighed just over one kilo and had very little chance of survival because she was premature and particularly small for her gestation.
"She wasn't able to maintain her temperature and was at high risk of infection because her immune system was low."
Ms Milroy and the other staff placed One Kilo (ultimately named Alicia) in space blankets and under heaters at night to keep her warm.
She was fed her mother's milk through a tube and given antibiotics but Ms Milroy said it was the tiny baby's "spirit and determination" that kept her alive.
Not all Ms Milroy's experiences were so fulfilling. She said sexual and other violence against women throughout Papua New Guinea was rife.
"One woman came in with machete wounds to her arms, chest and back after an attack by her husband - one wound was so deep on her arm, the bone was visible," she said. "I could help heal her wounds but I could not change her domestic situation."
Which is why Ms Milroy wanted to again work with MSF, which not only provides emergency care to those who live in areas of conflict or limited healthcare, but also training and education.