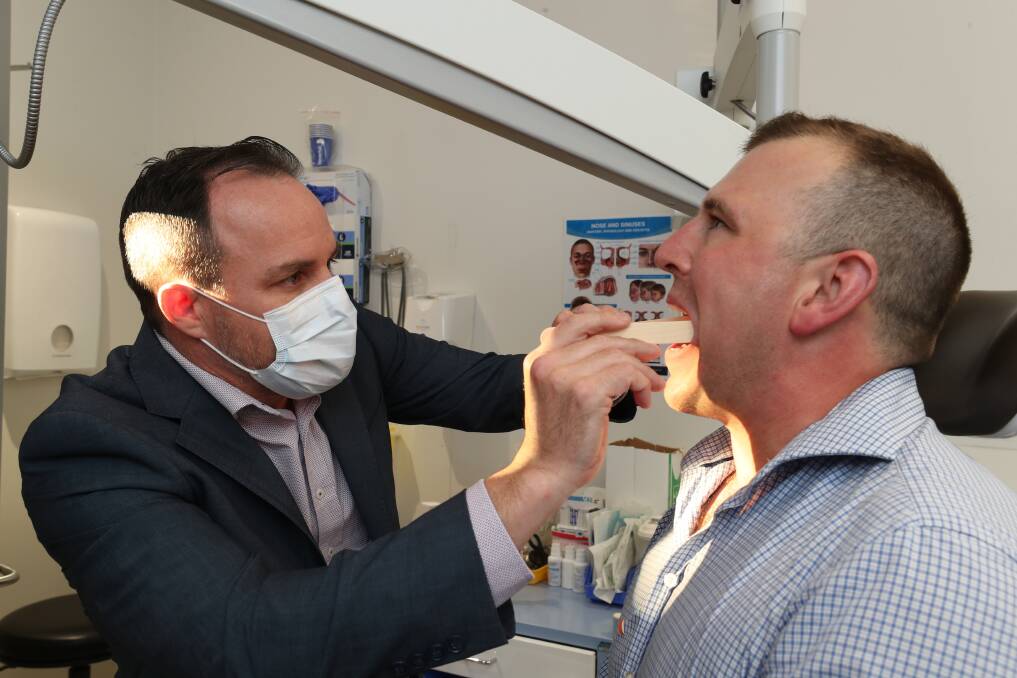
When Paul Richardson signed up to trial a pioneering surgery for sleep apnoea at Wollongong Hospital, it was after a decade of waking up tired.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
In his twenties, he'd put that down to partying, but after slowing down in his thirties, he knew there were other factors at play.
But he was amazed when a sleep study revealed his sleep was interrupted up to 30 times per hour due to stoppages in his breathing - sometimes for a minute or longer.
The Sydney man was one of 51 patients with severe, obstructive sleep apnoea to undergo the multi-level surgery that is now being promoted around the world after a successful trial at six sites across Australia, including Wollongong.
Forty of the 102 trial participants were treated at Wollongong public and private hospitals by Wollongong ear, nose and throat surgeon Stuart MacKay.
"It was a randomised trial, so half had surgery and half were given best medical advice to treat the condition - such as weight reduction, less alcohol and smoking cessation," Professor MacKay said.
The University of Wollongong honorary clinical professor was the lead manuscript author of the trial, which was recently published in the prestigious Journal of the American Medical Association.
"One billion people worldwide have obstructive sleep apnoea, yet 50 per cent of them cannot tolerate a CPAP (continuous positive pressure airway) mask," Professor MacKay said.
"This trial shows that surgery is a really important second line therapy that gives these patients another option.
"Because if untreated, severe sleep apnoea is associated with numerous adverse effects including problems with daytime functioning due to excessive tiredness as well as reduced quality of life. Longer term, there's an increased risk of cardiovascular issues including high blood pressure, heart attack and stroke."
Professor MacKay said the surgical technique combined a new version of palate surgery with a low risk tongue procedure, and tonsil removal if needed, to open up the patient's airway.
After six months, those receiving the surgery had an approximate 60 per cent decrease in the frequency of throat obstructions at night compared with a 20 per cent decrease in participants who remained on medical treatment.
"Obstructive sleep apnoea in adults is characterised by repetitive stoppages or droppages in air flow, often leading to oxygen droppage," he said.
"The key finding of this study was that this particular combination of surgical procedures led to a significant reduction in the number of breathing stoppages and droppages overnight.
"Patients also reported significant improvements in daytime sleepiness and a marked improvement in quality of life."
Professor MacKay said one of the major symptoms of sleep apnoea was snoring, though not all snorers have the condition. It's more common in men, and a formal sleep study is needed for diagnosis.
"I'm not a snorer and the only symptoms I had was waking up tired every day," Mr Richardson said.
"After my diagnosis I tried the CPAP machine, but didn't want to be dragging that around with me for the rest of my life.
"Plus it wasn't comfortable and I'd end up pulling it off in the middle of the night so it was ineffective anyway.
"After getting over the surgery, I found I had a new lease on life and a follow-up sleep study in January confirmed everything is now normal."
Another happy customer is Wollongong man Samuel Barlow, who underwent the surgery after the formal trial.
"I didn't have sleep apnoea but I've always snored which was a nuisance to me, and others who I've lived with, and left me tired all day," he said. "Since the surgery I've stopped snoring completely."
Professor MacKay was one of seven surgeons to perform the surgery across the six sites in NSW, SA and WA.
The trial was the brainchild of the late Professor Nick Antic, a Flinders University and SA Health respiratory and sleep specialist, who led the study until his death in 2016.
The trial, which ran from 2014 to 2017, was funded by the Australian government, Flinders University and the Repat Foundation.
Professor MacKay also thanked the Illawarra Shoalhaven Local Health District, Ramsay Health and the University of Wollongong for taking part in the collaboration, as well as other national and international partners.
Read the full paper here.
We depend on subscription revenue to support our journalism. If you are able, please subscribe here. If you are already a subscriber, thank you for your support.

