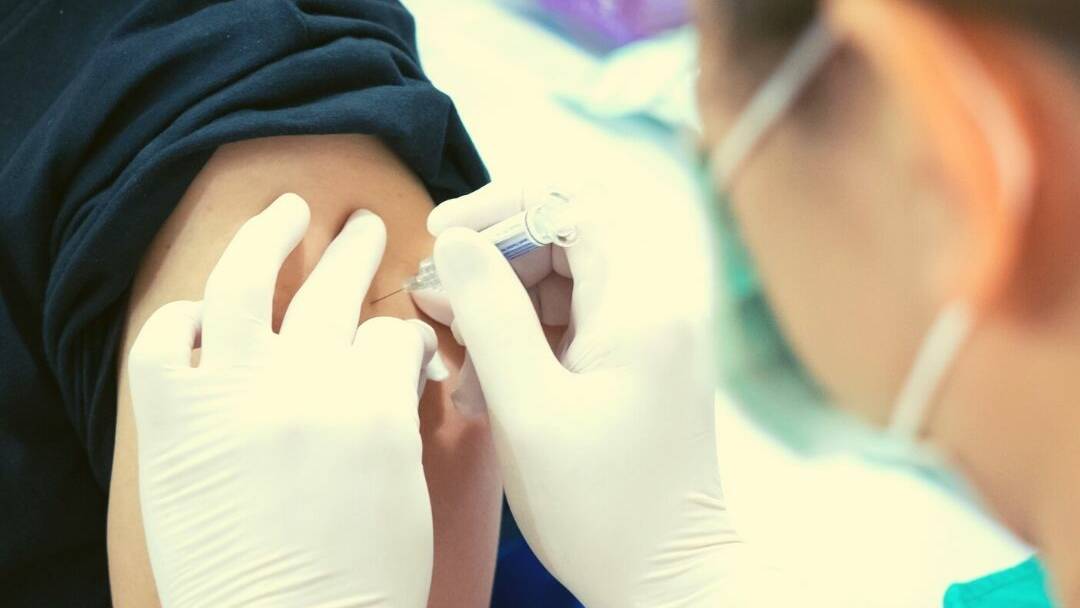
The COVID-19 vaccine rollout "is a race" says the CEO of one of the Illawarra's largest providers of aged care - and it's a race that the nation is far from winning.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Warrigal CEO Mark Sewell was responding to comments from Acting Prime Minister Michael McCormack on Sunday, who defended the slow rollout by insisting it was "not a race" - repeating earlier comments by Prime Minister Scott Morrison.
Around 500,000 Australians have received two doses of a COVID vaccine - which equates to just 2.5 per cent of the population. By comparison around 41 per cent of Americans, and 38 per cent of those in the UK, are fully vaccinated.
But it's not a race against other countries said Mr Sewell, it's simply a race to protect Australians - particularly the most vulnerable - especially coming into winter.
"It is a race," Mr Sewell said. "We need to have Australians vaccinated at a high level as soon as possible.
"It's vital - not just for the most vulnerable people who may die if the virus escapes into the community, but for people who have chronic illnesses who may suffer symptoms for a long time.
"We are now headed into winter with a largely unvaccinated population. It's a considerable worry for the health and community service sectors in Australia."
Mr Sewell praised the Federal Government's rollout of the vaccine for aged care residents, however he said that many aged care workers had been left behind.

At Warrigal - which operates 11 residential aged care homes across the Illawarra, Southern Highlands and ACT - around one in five workers are fully vaccinated.
On Tuesday Federal Aged Care Services Minister Richard Colbeck confirmed just over 31,000 aged care workers nationally were fully vaccinated. Mr Sewell estimated the total aged care workforce to be around 300,000.
"In March, aged care residents and staff were prioritised for phase 1A of the national rollout, and the plan was for vaccination teams to go out to every home and vaccinate residents and staff," he said.
"Staff were then dropped from that plan and the focus was put on residents, which was of course understandable as they were the most vulnerable.
"However unless staff were offered leftover vaccine from those visits, the teams did not come back for them and instead they have been asked to book in at hospital vaccination hubs or GPs.
"So while 90 per cent of our residents have been vaccinated, just 15 to 20 per cent of our staff have been vaccinated. From what I've heard that's pretty typical of most aged care homes."
Mr Sewell said surveys conducted internally also revealed that due to the slow pace of the rollout, vaccine hesitancy had set in.
"If you want everyone to do something, you have to make it simple - and that hasn't happened," he said. "Due to the delayed rollout, and changing advice, staff have lost confidence in vaccines.
"We conducted a survey a few months ago and 90 per cent of our staff said they were eager to have the vaccine, we repeated the survey last week and less than 60 per cent said they were eager to have it."
The outbreak in Victoria - which has found its way into aged care homes via staff - showed how vulnerable the nation still was, he said.
The Victorian government announced on Tuesday it will fast-track vaccinations for aged care and disability workers, with a five-day blitz from June 2 to 6.
However University of Wollongong's new Vice-Chancellor, Patricia Davidson, also has concerns about the Australian rollout after recent experience in the US.

Professor Davidson is back in the country after an almost eight-year stint as Dean of the School of Nursing at John Hopkins University in Baltimore.
"To be able to reach the numbers we need to get herd immunity, we have to have a coordinated vaccination strategy," she said.
"I see a lot of confusion here, with people not knowing where to go, or having trouble getting an appointment.
"The role of GPs is critical in coordinating care, yet to really get to the level we need to be at, it's really important we move more to mass vaccinations.
"In the US, vaccination teams were going to nursing homes, to housing complexes, to where people live. And there was a feeling that we're all in it together - that none of us going to be okay, until we're all okay."
Professor Davidson said she'd also witnessed vaccine hesitancy to a far greater degree than in the US.
"I think it's partly because people don't see COVID around them, they don't see there's a risk," she said. "Whereas in the US the suffering from COVID is so immense that people are just clamouring to get the vaccine.
"I think some people have also been made to feel they have a choice over what vaccine. In the US, the thought was the best vaccine was the one you could get on the day."
Do you have a story or news tip to share? Email us on cos@illawarramercury.com.au
Professor Davidson said high rates of vaccination could mean an end to border closures and lockdowns, such as the current situation in Victoria.
"What's happening in Victoria underscores the fragility of where we're at with this virus that's circulating," she said.
"Vaccination is so critical to really get to opening up our economy, to opening up our nation. Fortress Australia would be a good strategy if we weren't relying on global trade."
Universities of course are keen to see the return of international students, and Professor Davidson said there were benefits for all students, staff and researchers.
"I'd encourage anyone eligible to get the vaccine," she said.
"Having borders open is important not just for international students wanting to come back to study, but also for domestic students who want to travel overseas or take part in exchange programs."
Meantime an elderly Woonona resident, Elsa Story, rang the Mercury this week detailing her frustrations in trying to book a vaccine.

"I'm keen to get the vaccine straight away but could only make a booking for mid-July as my GP only gets a certain amount of vaccines each week as there's not enough supply," she said.
"We're being told to 'go and get your jab' but then there's delays. It means I wouldn't get my second dose until September. I'd prefer to be fully vaccinated during winter."
Ms Story, 77, said she wanted to get vaccinated not just for herself, but out of "social responsibility".
"I feel like it's a good thing for the majority of people to get vaccinated for the sake of the community," she said. "But I wish they'd make it a bit more accessible."
We depend on subscription revenue to support our journalism. If you are able, please subscribe here. If you are already a subscriber, thank you for your support.

