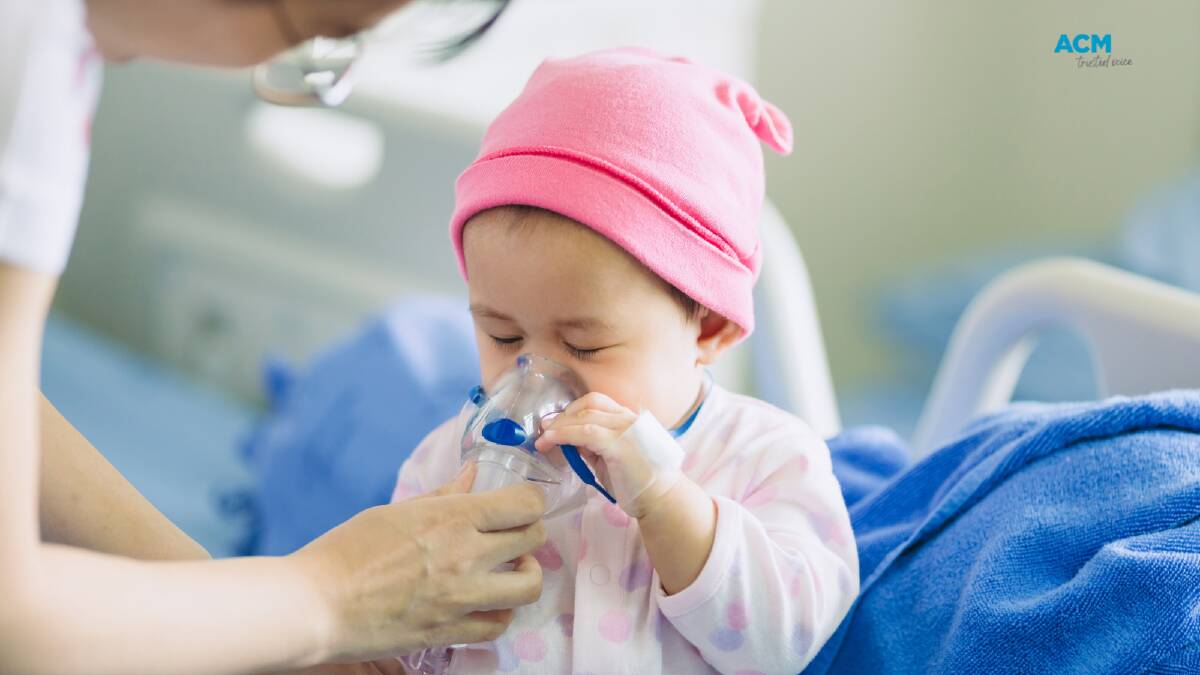
Medical researchers have started a project designed to treat sick outback kids near where they live - keeping them close to home and family, and saving millions of dollars in aeromedical transport costs.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Ms Sally West, a clinical nurse, researcher and PhD student at James Cook University's Murtupuni Centre for Rural and Remote Health, is part of a study that includes researchers from Griffith University, James Cook University, Wesley Hospital and Metro South Hospital and Health Services.
She said the team would focus on the treatment of children suffering Acute Respiratory Failure in rural and remote areas.
"Acute respiratory distress in children is the most common reason for emergency department presentations in Australia and is the reason for more than half of all hospital admissions of children under one year of age," she said.
"It's also the most common reason for paediatric aeromedical transfers in remote Australia."
Lead researcher Associate Professor Donna Franklin from Griffith University said many rural and remote hospitals see delays in transfers due to the distances involved, availability of aircraft or weather, often resulting in an extended stay in the local ED for the children and increased pressure on local resources.
IN OTHER NEWS:
"What we are setting out to do is introduce NHF therapy to rural and remote hospitals,'' she said.
She said the team had successfully trialled the introduction of NHF, involving training hospital staff in assessing the patient and increasing communication across rural to tertiary sites in three remote settings.
And now with a new grant of more than $1.6 million from the Medical Research Future Fund's Emerging Priorities and Consumer Driven Research Initiative, they would roll it out to 15 more.
"This will remove the need for many children to require aeromedical retrieval to main centres or spend extended times in EDs," Ms West, based at Weipa on the Cape York Peninsula, Queensland, said.
"It eases the pressure on stressed rural and remote EDs and we estimate savings at more than $6 million a year.
"Perhaps most importantly, it keeps children near their families and homes."
She said approximately 47 per cent of First Nations people live in rural and remote regions, with Aboriginal and Torres Strait Islander children, especially in remote communities, having a higher incidence rate of ARF than non-Indigenous people.
"A child and parent can be flown up to 900 km away into a hospital environment.
"In the case of Indigenous families, the significant cultural differences between staff and families contributes to feelings of powerlessness, fear and isolation.
"Indigenous communities have repeatedly reported the importance of receiving care on country and accelerating this trend will be a major goal of this work."
Ms West said the next phase of the project would begin in October and run to the end of 2027, with participating rural and remote hospitals implementing the NHF therapy independently by mid-2026.

