
A newborn with breathing problems who waited for five hours surrounded by coughing flu patients.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
An 82-year-old with sepsis whose daughters tried to make him a bed from seats and footstools while he was in emergency for 33 hours.
A five-year-old screaming in pain whose parents made the decision to take her home after she hadn't been seen by a doctor after seven hours.
These are a handful of the everyday stories that have come from patients who were in Wollongong Hospital's emergency department (ED) last week, amid growing concerns from doctors, nurses and paramedics about the hospital's capacity to cater for sick people in the region.
Shellharbour MP Anna Watson has also shared her own experience after spending most of the weekend in the ED supporting a cancer patient.
"Someone very close to me, who had stage four cancer, sat in ED for 10 and a half hours, and he was then told there were no beds," she said.
"They couldn't even find him a bed within the ED itself. There was not enough seats for the people who were in there, there were ambulances queued up out the back.
"There were so many babies and infants with this awful whooping cough-type cough and they were having to wait. Someone had a big vomit right in front of me at my feet.
"I felt like I was in some cheap American low-budget clinic, and it really frightened me that here I was in NSW in the Illawarra in 2022 and this is what I was seeing."
She said the person she was with in hospital ended up leaving out of frustration and exhaustion.
"This person I was with got very agitated, upset, anxious, tied and sick, because that's how you feel with stage four cancer," Ms Watson said.
"It got to the point where he finally did get put into a little tiny bed in a consulting room with another patient, spent the night there and then the next day got his son to come and drive him back to his nursing home because he couldn't stand it anymore.
"I begged him not to go, because that means he's not going to get the treatment he needs."
'There were so many kids! It was heartbreaking.'

Fairy Meadow mum Tylah Buckley spent three days in the children's ward last month with her newborn daughter Mahli, who had contracted respiratory syncytial virus (RSV) when she was two weeks old.
Mahli improved but still had "a horrid cough" when she left the hospital, and Ms Buckley said she was doing okay until last Sunday, when she was choking on mucus, fussing to feed and her coughing and breathing was getting worse.
On Monday, she took Mahli to the GP, who sent them to emergency.
"Both the nurse and the GP took one look at her and said she needs to go straight to emergency to be monitored closely," Ms Buckley said.
"He wrote me a referral which had 'urgent' written on the top with all the details including her colour change when coughing, her low saturations, distress and pneumonia."
They arrived at 10am, and before being triaged they sat in the only chair available which was next to a child whose mother said he had influenza.
"I kept the blanket over her in her pram and was wishing it would be quick so I didn't have to get her out in the open with so many other sick people," Ms Buckley said.
"A few hours later I addressed my concerns to the triage nurse saying I was worried [about] my baby having to be in the waiting room with everyone around us so sick, and all she could suggest was a mask over Mahli's face as the isolation area was full of COVID positive patients."
"There were so many kids! It was heartbreaking."
Five and a half hours after their arrival, Mahli was seen by a doctor, who told Ms Buckley she'd be best to take her home.
"He had a little look at her and said her visual observations look ok and if she is day two of this new sickness, three and four are the worst so keep her at home and bring her back when she gets worse. He assured me if I came back up again she wouldn't have to wait again and would be seen quicker."
"Obviously I was already concerned about having her in there and I wasn't being closely monitored like my GP had initially said so I thought taking her home would be more comfortable."
"I spoke to my doctors surgery who were shocked they sent Mahli away, and booked her an appointment in 24 hours to be seen again."
"I have been advised by numerous people with similar situations to skip Wollongong and go straight to Westmead Children's."
'Our daughters tried to make him a bed on the seats and footstools'
The wife of an 82-year-old Towradgi man has shared her family's experience over the weekend, after her sick husband was stuck trying to sleep on footstools during a 33 hour wait in the ED.
The woman, who has asked to keep her name private, said her husband had been a frequent visitor to the hospital in recent times, but that they have never seen it as bad as it was during their multi-day visit.
"I know the staff are working hard, but something has to change," she said.
On Saturday around 8.30pm, he was showing signs of infection after a medical procedure and had been told to get to emergency immediately if that occurred as it could be the potentially deadly condition sepsis.
"We rang for an Ambulance and after much screening they advised we would be better to go by our own means even though he had a catheter," she said.
On arrival at 9pm, he was triaged within 10 minutes and sent back to the ED waiting room, before being seen by a nurse and having blood taken for tests which came back positive two and a half hours later.
"Overnight he was monitored and had regular changes of IV and was advised he had been admitted, however there were no beds, so we continued to sit in the ED waiting room with many other patients," she said.
"The nurses continued to monitor him by administering IVs, they were doing their best, under very difficult circumstances."
While he waited for a bed in a ward, along with at least four others waiting to be admitted, she said they had little access to food or drinks.
"Around 6.00am he was brought a box with "breakfast," no water or tea/coffee. I went home several times during the day and overnight making thermos' of tea and taking snacks," she said.
"All day this continued until around 8:30pm when our daughters tried to make him a bed on the seats and footstools in the waiting room because he was continually dropping to sleep and almost falling off his chair.
"He has many other medical problems."
The man was eventually able to go and lie on a bed, when staff from another ward were brought in to supervise, and was admitted to the hospital early on Monday morning, 33 hours after his arrival.
Share your story: Why we need to share your experiences at the Wollongong Hospital ED
'They were unable to see a 5 year old child crying and grabbing at their stomach inside 7 hours'
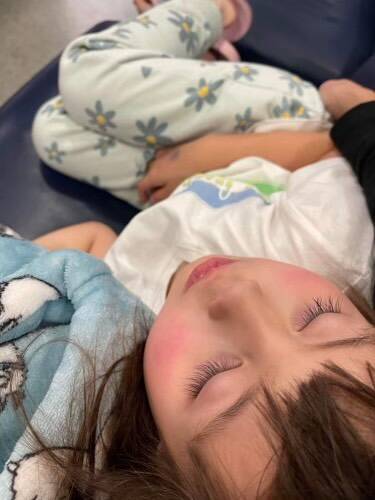
Figtree dad Robert Sharpe says he would look to hospitals outside the Illawarra after his experience at Wollongong ED last week.
After complaining of a sore stomach last Wednesday evening, his five-year-old daughter Jessica was " crying nonstop and grabbing at her stomach in extreme pain" by 9pm.
"We wasted no time in going straight to emergency at Wollongong hospital, arriving not long after," Mr Sharpe said.
"The waiting area was near full (with audible complaining from everyone about how slow things were). We saw a triage nurse within about 15 minutes of being there and assumed a crying child in visible pain, grabbing at their stomach would be seen relatively quickly."
At 2am, the family was told the paediatric areas was full but that they were next. By 3.30am, thinking it was not going to be possible to be seen by a doctor, Mr Sharpe decided to take Jessica home.
"[We thought Jessica was] is safer in bed than a room full of sick people and if the problem comes back we will call an ambulance and take our chances with that," he said.
"The next day we went to a GP who advised us to go straight to the emergency section at Wollongong hospital on the spot. He wrote us a letter that he insisted would get us in quicker but we told him full means full, it's not because triage is slow."
Fearing that Jessica had appendicitis, the GP organised an emergency ultrasound from a local clinic to rule that out.
Mr Sharpe said he was concerned about the Wollongong ED's ability to cater for the growing population of the Illawarra.
"I moved down to Wollongong about four years ago from Sutherland," he said.
"I have noticed the large amount of cranes on the skyline and the addition of a number of larger apartment buildings creating a lot more newer dwellings. Unless there is greater interest and work on making the system more functional, the issues we faced will only get worse.
"All of the staff seemed tired and exhausted. They go to work each day knowing the system isn't at breaking point, it's broken. They simply cannot provide medical services to meet the demands as enough are not available."
"At present a five year old crying in pain grabbing at her stomach couldn't even get in a room with a doctor inside 7 hours - and who knows how long it would have been if we continued on."
He said he would either call an ambulance or drive to Sutherland for emergency treatment in the future.
"The main thing I would like to have known is that the place was full earlier on," he said.
"It's not a case of continuing to wait as people are no longer being processed until someone leaves and it takes a long time before a child would be discharged. We could have tried an alternate hospital if there was an availability somewhere else."
We are asking Mercury readers to share their stories - good and bad - to add voices to the views of staff who have been raising the alarm about what its like working in our hospitals for months. You can add your experience by filling out the form below.
A statement from an Illawarra Shoalhaven Local Health District spokesperson:
The Local Health District reassures the community that our hospitals and emergency departments (EDs) are open 24 hours a day, 7 days a week, 365 days year.
We activate well established workforce surge and demand management plans during periods of high demand, including increasing bed capacity in hospitals where possible, ensuring all available clinical staff are deployed to the care areas with the highest demand, and improving the timeliness of patient discharges with appropriate community follow-up support where required.
We also have dedicated initiatives in place, including teams focused on timely access and the safe flow of patients through our hospitals at all times.
Wollongong Hospital has been experiencing high demand for emergency care and patient admissions in recent months. At the same time, teams have been managing the impacts of COVID-19, including the unavailability of staff due to illness.
Despite these challenges, our dedicated staff continue to work incredibly hard to ensure that patients who present to the ED with serious and life-threatening conditions, like heart attack and stroke, will always be seen immediately. With the support of our NSW Ambulance colleagues, we work collaboratively to ensure all patients are seen and treated as quickly as possible.
Regardless of the mode of arrival to ED, all patients are triaged and seen by a doctor according to the seriousness of their condition. This means that patients with less urgent conditions may need to wait longer during periods of high demand, even those arriving via ambulance.
We ask that our community considers alternative options to the ED for minor conditions. These options include medical centres or GPs, the Urgent Care Centre at Bulli Hospital, pharmacies or calling HealthDirect on 1800 022 222; a 24-hour telephone health advice line staffed by registered nurses who provide fast and simple expert advice.
If the situation is life-threatening, always call Triple Zero (000) immediately go straight to the Emergency Department.


