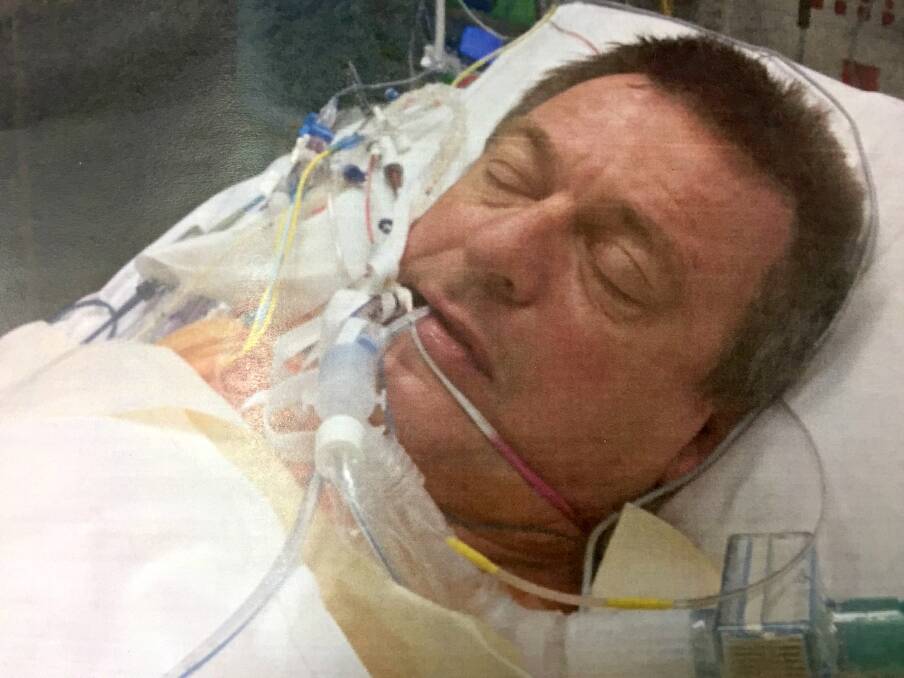
Alan Teall fears he won’t make it to his 70th birthday.
Subscribe now for unlimited access.
or signup to continue reading
The 60-year-old Tomerong resident contracted Q fever in late 2015.
At the time, Mr Teall, 60, was running a property maintenance business in the Sanctuary Point region. He unknowingly breathed in kangaroo faeces while mowing a lawn.
In April last year complications from the disease saw Mr Teall suffer a heart attack and later undergo open heart surgery. A cow’s valve was used to replace his damaged mitral valve.
Mr Teall will need another heart replacement operation in 10 years time but fears he will not live that long.
“I'm the healthiest person on the planet who got to be the sickest ,” Mr Teall said.
“The Q fever bacteria could attack the cow’s heart valve over the next three to five years. It’s not guaranteed to happen but if it does, it will kill me.”
Mr Teall said he wasn’t aware of Q fever and is concerned with the lack of education surrounding the disease, on behalf of NSW Health.
Before undergoing surgery, he said he was contacted by a NSW Health representative who told him the region he contracted the disease was one of four Q fever hotspots in the Sanctuary Point region.

“Why isn’t this information out there?” he asked.
“I was told there’s been a vaccine out for Q fever for 20 years but if you don’t know about it, you’re not going to go looking for it.
“There needs to be more awareness and attention on this so it doesn’t keep happening to anyone else.”
NSW Health released a statement in response to Mr Teall’s claims and said the NSW Government has committed $200 000 for a new statewide communication strategy, developed with input from NSW Farmers and other stakeholders, to educate rural and regional communities about Q fever.
“NSW Health is also partnering with the Australian College of Rural and Remote Medicine to develop an education package to up-skill rural and regional GPs on preventing, diagnosing and treating Q fever,” a NSW Health representative said.
“While people in some specific occupations are at increased risk of Q fever, Q fever can affect anyone exposed to infectious animals.
“NSW Health is working to collect better information about notified cases to better target groups now emerging in NSW as at risk of Q fever.
“As we learn more about emerging risk groups we will be working with GPs to tailor our messages to these groups.”
NSW Health advised they are pushing for national funding for more Q fever research.
Mr Teall hasn’t been able to work full-time since his diagnosis. He said his family's finances have been taken a hit and he requires constant medical supervision.
“I’m a physical and emotional wreck,” he said.
“We need to raise awareness of this disease, I’ll do whatever I can to stop this happening to someone else.”
Find more information about Q fever here and for identified notifications of Q fever in Illawarra and Shoalhaven residents head to www1.health.nsw.gov.au
Q fever – what you need to know
About
Q fever is an infection caused by Coxiella burnetii, a type of bacterium found worldwide except New Zealand. The infection is almost always related to direct or indirect contact with animals such as cattle, sheep or goats, although a wide range of animals including cats, dogs and kangaroos may carry the infection. Infection in animals is probably common, but animals usually do not appear to be ill.
How Q fever is spread
Infection of humans usually occurs by inhalation of the bacteria in air carrying dust contaminated by dried placental material, birth fluids, urine or faeces of infected herd animals.
Signs and symptoms
- fever, which may last for up to four weeks
- severe headache
- sweats and chills
- fatigue – and a prolonged fatigue (post Q fever fatigue syndrome) may follow infection
- muscle aches
- confusion
- sore throat
- dry cough
- chest pain on breathing
- nausea, vomiting
- diarrhoea
- abdominal pain
Some people may develop chronic Q fever after exposure. Infection persists for more than six months and may not be apparent until many years after the initial infection. It is rare, but can have serious complications such as endocarditis (infection of the heart valves).
Diagnosis
Diagnosis is made by a series of blood tests.
Incubation period
Usually two to three weeks, range four days to six weeks.
Infectious period
Person-to-person spread occurs rarely.
Treatment
Effective antibiotic therapy is available. With early diagnosis, treatment is simple and a good outcome can be expected.

