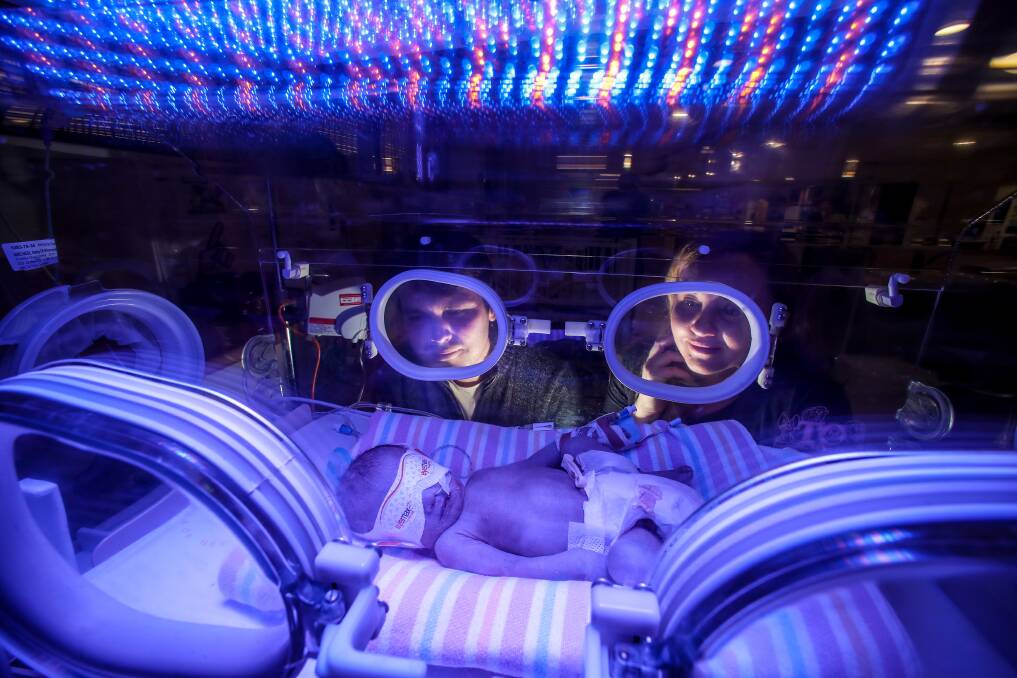
Seeing their first-born child struggle to breathe after being born six weeks premature this month was devastating for Corrimal parents Jonathan and Blacenka Archer.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Thankfully staff at Wollongong Hospital's neonatal ward were fully equipped to help their tiny boy breathe easy, having taken part in a landmark study into the most effective methods of respiratory support for preterm babies.
"My wife needed a Caesarean at 34 weeks due to preeclampsia, and I just broke down when I saw our little boy come over the curtain (in the surgery)," Mr Archer said. "Watching his little rib cage nearly bursting as he struggled to breathe was one of the hardest things."
The Hunter trial, published this week in the prestigious New England Journal of Medicine, was led by the Royal Women's Hospital in Melbourne and involved nine non-tertiary hospitals in NSW and Victoria, recruiting more than 750 preterm babies in special care nurseries between 2015 and 2017.
It looked at whether a simple and more gentle breathing support - nasal high-flow therapy - could be used instead of, or in conjunction with, the well-established breathing support of nasal Continuous Positive Airway Pressure (CPAP).
Professor Ian Wright, who led the study at Wollongong Hospital, said the study was unique in that it was conducted out in several smaller, non-academic hospitals where newborn clinical research was not commonly carried out.
The majority of babies born at 32 weeks and above are cared for in such hospitals, so the trial has given neonatal staff clarity on how to best support the breathing of their tiny patients.
While Wollongong Hospital has access to CPAP, nurseries at some smaller hospitals did not which meant that preterm babies often needed to be transferred to larger hospitals.
"The study looked at the way we support babies who have breathing difficulties soon after they're born," he said. "The main idea was to see if not only could we stop the babies from getting sicker, but whether we could also prevent them needing transfer to larger centres - allowing them to stay in hospitals closer to home."
Prof Wright, a professor of paediatrics and child health research at the University of Wollongong, said there were other benefits to trialing nasal high flow therapy.
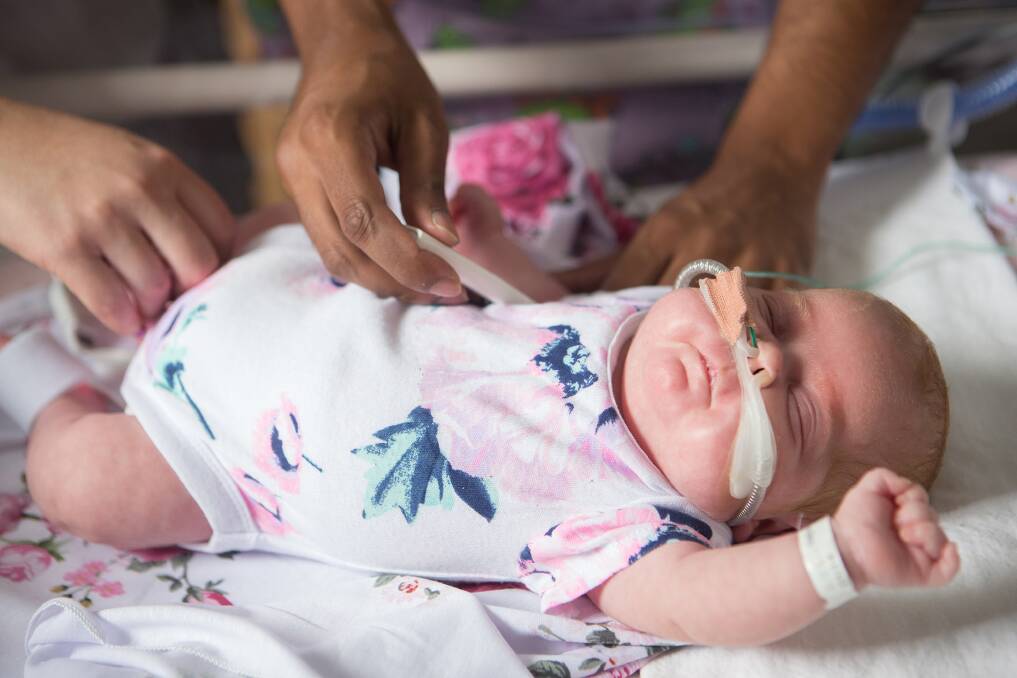
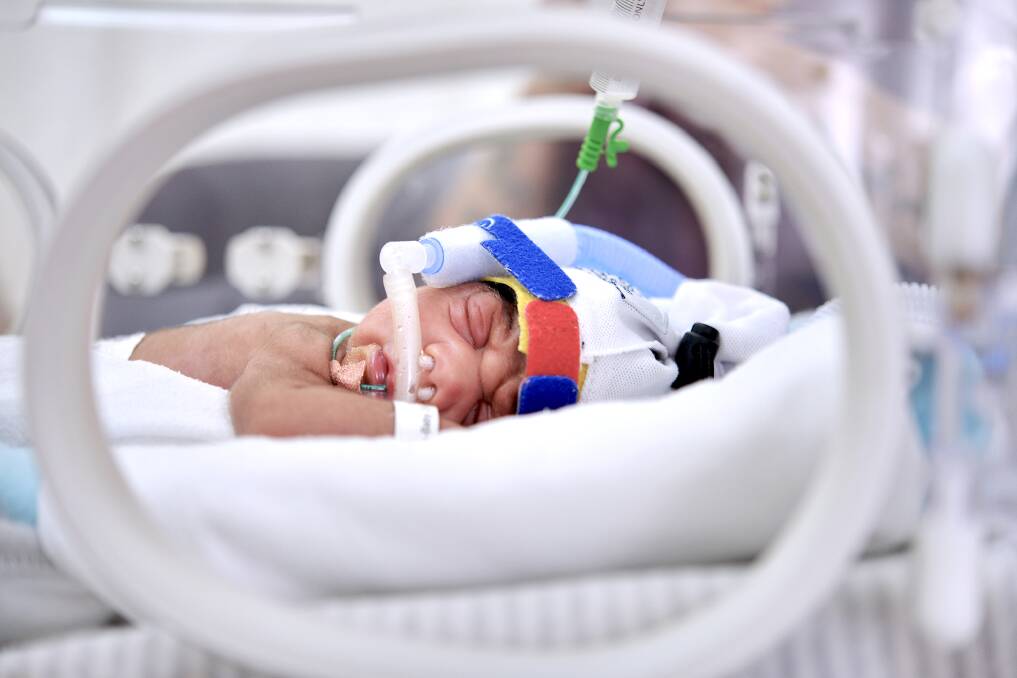
"It uses small prongs placed in the baby's nose and attached to their cheeks, rather than CPAP which uses larger prongs fitted in the baby's nose and tubing that's strapped to a special hat," he said. "High flow is a simpler system and more comfortable for babies, and allows parents greater freedom to cuddle and care for their baby."
While the study found that CPAP was still the better respiratory support for some newborn infants, in about 80 per cent of the babies high-flow worked well and they didn't need any other breathing intervention.
For little Edward Archer, with a birth weight of 1.7kg, CPAP remained the best option. "Soon after he was attached to the machine, we could see him breathing gently," Mr Archer said.
Dr Susie Piper, co-director for paediatrics, said the study gave staff the knowledge of when it was safe to use the gentler high flow method.
She thanked staff, including neonatal nurses Ashley Blood and Patrice Nolan, for their hard work in implementing the trial which was funded by a National Health and Medical Research Council (NHMRC) grant.

