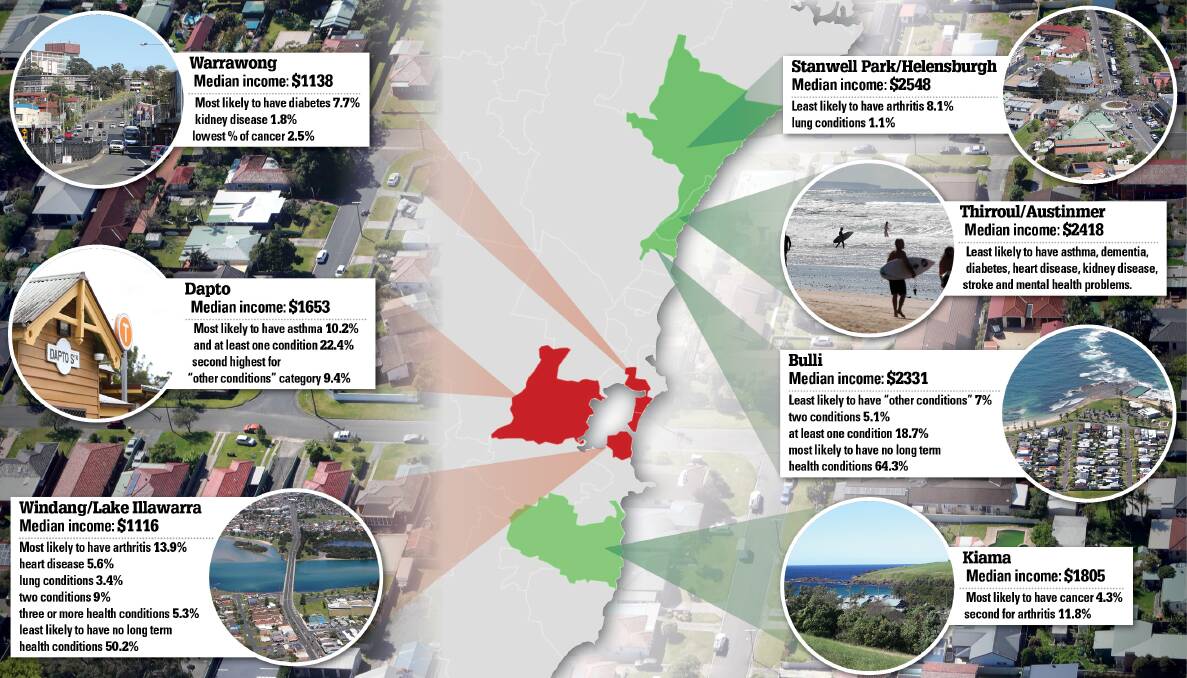
Where you live in the Illawarra could have a big influence on your health, with figures showing a striking divide between rich and poor areas when it comes to chronic health conditions.
Subscribe now for unlimited access.
or signup to continue reading
An analysis of Census data comparing income with the prevalence of ten different long-term health conditions shows that, in most cases, suburbs with a higher median income were less likely to be sick.
The reverse was also true, with the poorest suburbs more likely to have conditions like heart disease, diabetes, lung conditions, kidney disease and mental health problems.
Residents in Bulli, the region's third richest postcode, were the least likely to have a chronic health problem with 64.3 per cent reporting no long term health conditions.
But at the other end of Wollongong, in the 2528 postcode that bridges Windang, Lake Illawarra and Wariila and has the second lowest median income, only half the residents said they did not have a chronic health issue.
In Thirroul, which has a median income of $2418, residents are the least likely in the Illawarra to have asthma, dementia, diabetes, heart disease, kidney disease, stroke and mental health problems.
But in Warrawong where the average income in $1138 there are much higher rates of illness, with the postcode ranking worst for diabetes and kidney disease.
The suburbs with the lowest median income were also significantly more likely to have complex health needs, with more people reporting two, or three or more, long-term conditions.
The one condition which did not seem to discriminate based on income was cancer, with Warrawong having the lowest prevalence of cancer and Kiama, which has the region's oldest median age, having the highest.
Relatively affluent Woonona, which is ranked ninth out of 18 postcodes for income, is also a bit of an outlier: it had the highest prevalence of dementia and was second for arthritis, which could possibly be explained by the number of aged care homes within the suburb.
Health researchers and public health workers say the link between income and health is well-established, with the Australian Institute of Health and Welfare reporting that people in lower socioeconomic groups are at greater risk of poor health, have higher rates of illness, disability and death, and live shorter lives than people from higher socioeconomic groups.
"The higher a person's socioeconomic position, the healthier they tend to be - a phenomenon often termed the 'social gradient of health'," an AIHW report from 2021 said.
The higher a person's socioeconomic position, the healthier they tend to be - a phenomenon often termed the 'social gradient of health'.
- Australian Institute of Health and Welfare
"In countries at all levels of income, health and illness follow a social gradient: the lower the socioeconomic position, the worse the health."
Likewise, University of Wollongong public health researcher Associate Professor Tam Ha said it was "absolutely no surprise" that theIllawarra data showed a stark difference between those with a chronic disease in the high and low income postcodes.
"There's many different factors that influence our health, there's health care, individual health behaviours, the physical environment in which we live, and then there's socio-economic factors," she said.
She said socio-economic factors such as income, employment, housing and education were the highest contributing factor to a person's health, making up about 40 per cent of their overall health and well being outcomes.
"Income influences our health outcomes in a variety of different ways such as access to more timely treatment, choice of specialists and a wider range of treatment options," she said.
"Income also allows individuals to make healthier lifestyle choices such as choosing healthier (and often more expensive) food options and gym membership to name a few. It is also connected to factors like literacy, being able to take action, being able to navigate the health system and knowing when to change your lifestyle and behaviours."
She said it was easier for people on higher incomes to live a healthier lifestyle.
"A lot of chronic diseases can be prevented, so diabetes, cardiovascular disease and even cancer can be prevented to a large extent," she said.
"If you're not worried about how much money you spend on food, for example, you can buy healthier food. But if you are struggling to pay the rent and the bills, fast food is generally a bit cheaper.
"If you are struggling to make ends meet - working multiple jobs - then you're not going to prioritise exercise, diet, etcetera, and when life gets too tough, you're not going to quit smoking or quit drinking."
Despite prevention making a big difference, Prof Ha noted that only a tiny portion of the health budget - less than two per cent - was spent on prevention and said this was vital to take the pressure of the more expensive spending needed to allow hospitals to cope with higher health needs.
More prevention funding needed

CEO of non-government organisation Healthy Cities Illawarra Kelly Andrews said she would also like to see more money going into prevention.
"These things we are talking about are chronic disease, they build up over decades and end up costing the public health system a lot of money," she said.
"The problem is, by the time you get into the health system, there is an issue with your health - and what we really need to keep people healthy is preventative stuff: the basics of housing, education, access to food, clean air."
"It's a brave person who would say we shouldn't be spending so much on the hospital system and ambulances, and we certainly need those services, but health prevention is the most marginalised. It's a no brainer, that if you can keep people well outside of the health system, they are more likely to maintain better health in the long run."
Ms Andrews said her organisation ran numerous grassroots programs which have been helping to change things for people in disadvantaged areas. However she said these struggled to attract ongoing funding.
"As an example, we have a program called Cook Chill Chat and we've just lost federal funding for that," she said.
She said the program helped women escaping domestic violence, Aboriginal groups, multicultural communities, refugees and new migrants to learn about nutrition, eating on a budget and reducing food waste.
"It's a well-established program, evidence based program meeting a lot of vulnerable people with excellent and sustainable outcome to support their health, but now it can't continue," she said.
"So we need prevention and health promotion to be better funded, because we simply cannot keep funding hospitals because we can't afford it."
The Census data also shows that Illawarra residents are sicker and more likely to have long-term health conditions than Australia and NSW.
For instance, only one Illawarra suburb - Thirroul - has a lower rate of asthma than the general NSW population, and in every illness category the prevalence of disease is higher in the Illawarra than for NSW and Australia.
What's being done to help change things?
The region's health boss Margot Mains said the Illawarra Shoalhaven Local Health District used data, including that from the Census, to plan and deliver health services to at-risk populations across the region.
"We know vulnerable people and those with high social disadvantage are at higher risk of poor health due to the barriers they experience," she said.
"A population-based approach to our service planning allows the District to understand the causes of poor health and the areas with the highest burden of disease so we can deliver health related services with the greatest potential to improve health."
She said the $700 million new Shellharbour Hospital was being planned with the future health needs of the surrounding suburbs in mind, and noted the Shoalhaven Hospital Redevelopment would include a dedicated cardiac facilities in response to the higher level of cardiovascular disease in that area.
Ms Main said the district was also focused on helping people stay healthy through community-based and outreach services.
"Recently, we have seen the opening of new HealthOne Centres in Dapto and Ulladulla, with planning underway for the new Warrawong Community Health Centre," she said.
She said the district had targeted health related services supporting those with a higher burden of disease.
"ISLHD community health services provide care in clinics and people's homes across a range of areas including general and specialist nursing care, allied health services as well as counselling services, women's health, sexual health, chronic disease support and the diabetes service," she said.
"The LHD also runs community based programs for refugees, people from diverse cultural and linguistic backgrounds, the Aboriginal community, families and young people.
"The District also has a strong focus on prevention strategies and our Health Promotion programs and activities are targeted to communities and areas with the highest prevalence of chronic diseases and where they can have the biggest impact.
"Health Promotion works to help people make healthy living choices by providing a range of healthy eating, active living and smoking cessation programs."
We've made it a whole lot easier for you to have your say. Our new comment platform requires only one log-in to access articles and to join the discussion on the Illawarra Mercury website. Find out how to register so you can enjoy civil, friendly and engaging discussions. Sign up for a subscription here.


