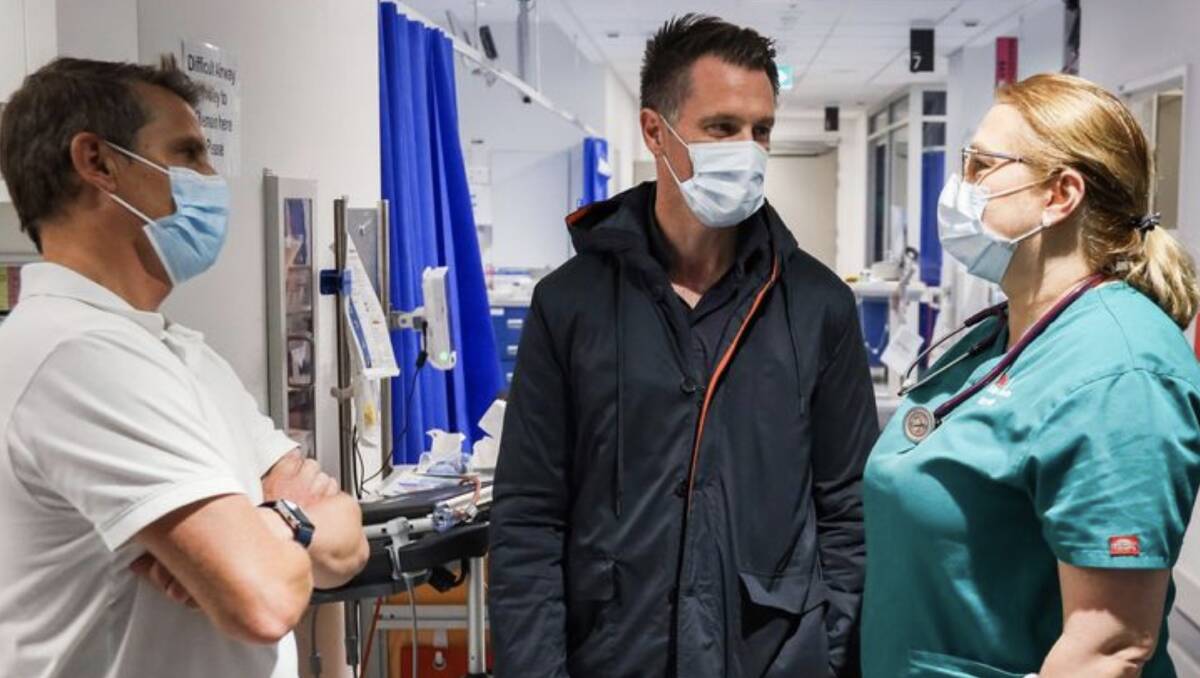
Just after midnight on Tuesday, Ryan Park and Chris Minns wandered the halls of Westmead Hospital, chatting to health workers about what needed to be done to fix the state's health system.
Subscribe now for unlimited access.
or signup to continue reading
In Wollongong emergency department at the same time, a sick intensive care nurse who needed treatment for a chronic illness was propped up on a plastic chair with a drip in, halfway through a 24-hour wait to get a bed.
As the new Premier and Health Minister tried to find solutions to the bed block, long waits in emergency and staffing crises that have plagued health in recent months, the local nurse - who works in Sydney and can't be named due to NSW Health's restrictions on staff speaking to the media - was living through the problem.
His partner, Georgia Holloway, from Bulli, said she was astounded at how bad the wait was at Wollongong.
"I was really upset because he is a registered nurse and he's dedicated going on 10 years of his life to care for other people,' she said.
"And then when he goes to receive health care, you have to wait 24 hours just to get a bed in the local hospital."
Ms Holloway said her partner arrived at the ED at 11.30am on Monday needing medication and to be admitted, and could not get into a bed until 11am Tuesday.
"It was 23 and a half hours waiting in the waiting room," she said.
"So those hard plastic chairs that you see at airports, he was sitting on one of those for 23 and a half hours.
"They would take him back to the triage bay and give him [intravenous] steroids and then send him back out to the waiting room."
Ms Holloway said it was so uncomfortable that she wondered at one point whether he could go home and wait, as being a nurse meant he may have been able to monitor his medication.
"I thought maybe they'll say come back in the morning and he could get into a bed then," she said.
"But they said, 'no, you've been admitted, sort of, even though we don't have a bed and now you're under our care so you cannot leave'."
"They said we literally have no available beds in this entire hospital. But thank goodness we finally got one, and I'd say he'll be in there for a few days at least."
Like most people who have experienced long waiting times, Ms Holloway said she had no problem with the staff or care given in Wollongong ED
"I just find it ludicrous that in 2023 in a country like Australia that the healthcare system can't even support its own workers," she said.
Ms Holloway said she would be watching closely to see whether Mr Minns and Mr Park listened to health workers and patients as they begin their new term of government.
Park's plan: snap visits to hospitals and an 'obsession' with fixing EDs
Speaking to the media after being sworn in to his new role on Tuesday, Mr Park praised the NSW Health system and its workers, saying fixing emergency departments would be his "obsession" and that there would be "no greater advocate for public health".
He announced he would be making snap visits to hospitals across the state at different times of day to learn what was going on at each facility.
"I want our focus to be on improvement," he said.
"We've got to try and take some pressure off emergency departments, [its] not going to happen overnight, but it is going to be something that I will have an obsession about to try and make it easier, not just for patients and their families, but also healthcare staff."
Mr Park noted that in Wollongong Hospital, there were currently 130 people who needed a place in aged stuck in hospital beds, and said he would need to work closely with federal health minister Mark Butler on Medicare reforms and making it easier for patients to see a GP.
"Every single week through my electorate office down in the Illawarra, I come across people who are struggling to get into GP books," he said.
"That's one problem and then we are starting to see a reduction in the number of GPs bulk billing, [and] that's exacerbated by a workforce that is ageing and starting to want to do other things after a very, very difficult few years.
"So we've got to look at every single possible way that we can make sure that primary health is sustainable, strong and robust because emergency departments were never meant to be GP clinics."
He said urgent care centres were part of the solution, but that he did not want them to just be doubling up on the work of EDs.
"You've got to be careful, they have to have diagnostics and that sort of thing inbuilt into them because what we don't want to see is just the movement between an urgent care centre and an ED so we're doubling up," he said.
"I've always said that they won't be the silver bullet, but nothing is the silver bullet here piece by piece, bit by bit."
New taskforce - and new words - to tackle surgery waitlist
As their first move after being sworn in, Mr Minns and Mr Park announced they had directed the health department to set up a "Surgical Care Taskforce" promised by Labor to tackle the state's 100,000-person waitlist for elective surgery.
Speaking at Liverpool Hospital, Mr Minns said 17,000 people - including 4000 children - had been waiting longer than recommended.
Mr Park said he expected a report back from the taskforce in three months and believed the term "elective" surgery should change.
"Everyone knows that COVID put a big dent into the ability for people to access surgery," he said.
"And from now on, I'm going to start calling it planned surgery. You'll note that in opposition, I didn't like the term elective surgery. It sounded like people had a choice.
"This is surgery that people are living in pain with, that they need to reduce the pain and suffering that they've experienced."


